By Rachel Schraer
(News investigators) How do you ask a community to trust medicine when history has given them many reasons not to?
It’s a dilemma US nurse Victoria Baptiste has to deal with every day as she travels around Baltimore County, Maryland, in a mobile clinic, administering Covid vaccines.
Over the past couple of years, one question has kept coming up, especially from her black patients. We’ve been experimented on in the past – how can we trust this treatment?
Often they’ve come across inaccurate posts on Facebook or Twitter. But her black patients’ fears have not just come from online misinformation – their mistrust began long ago.
“When they start to tell their stories they say, ‘Remember Tuskegee and Henrietta Lacks, they always experiment on people of colour,'” she says.
Tuskegee was a 40-year experiment conducted by the US government in which hundreds of black men were deliberately left untreated for syphilis, without their knowledge. After it was exposed, regulations were introduced in 1974 that required voluntary informed consent from all subjects taking part in research.
And as for Henrietta Lacks – few people are better placed than Victoria to understand that story of unethical medical research. Henrietta was the mother of Victoria’s beloved grandfather, Lawrence.
Henrietta Lacks was an African-American woman who died of cervical cancer in 1951 and whose cells were used for medical research without her or her family’s consent.
As she was being treated for her cancer, some tissue was scraped from Henrietta’s cervix into a petri dish, as part of a search for cells that could be studied and experimented on outside the body.
She wasn’t told this was happening. Nor was she kept fully informed about the effects of the treatment she was receiving for her cancer, Victoria tells me. She had radium – a radioactive substance – sewn into her cervix to try to kill off the tumour. It was an accepted treatment at the time, but she was not told that this could prevent her from having more children.
Meanwhile, where other cell samples quickly died despite scientists’ best efforts, Henrietta’s cells not only stayed alive – they multiplied at a rapid rate, leading them to be termed “immortal”.
The spiralling number of these cells, a feature of her cancer, would prove devastating for her – but revolutionary for science.
This stock of human cells can then be used to understand how diseases affect the body, and as a first testing ground for treatments, improving both the speed and safety of medical research.
Henrietta Lacks’s cells – dubbed HeLa – have been involved in understanding cervical cancer, tuberculosis, Ebola and HIV as well as laying the groundwork for polio, Human Papilloma Virus (HPV) and Covid vaccines.
They have benefited millions of people – and made potentially billions of dollars for the drug companies that use them to test their products. Yet the Lacks family has never seen a penny of these profits. At one point some family members couldn’t even afford medical insurance.
The full details about HeLa cells were only drawn to some of the family’s attention when science writer Rebecca Skloot, who wrote a best-selling book about the case, started investigating.
So when Victoria says she understands why people might be mistrustful of the pharmaceutical industry, she means it.
A nurse in the family
Victoria grew up hearing about the mother her grandfather Lawrence lost before he reached adulthood: a mother of five who cared for everyone and yearned for more children, and who loved to cook, dance, and make herself look nice.
Victoria and her posse of cousins – her best friends to this day – spent their early years running around the home of Henrietta’s husband David, known as Day. And it was really thanks to him that Victoria became a nurse in the first place.
“He had to live with diabetes when I was a young child, and I was always very curious and asking questions like, ‘Pop why are you giving yourself needles? And what is this for?’ And he was always very patient with me.” She eventually learnt to administer his insulin injections.
In early 2020, Victoria was working as a nurse in a hospital kidney unit. But when Covid hit, her work changed dramatically. Like many healthcare workers she was afraid of taking the disease home.
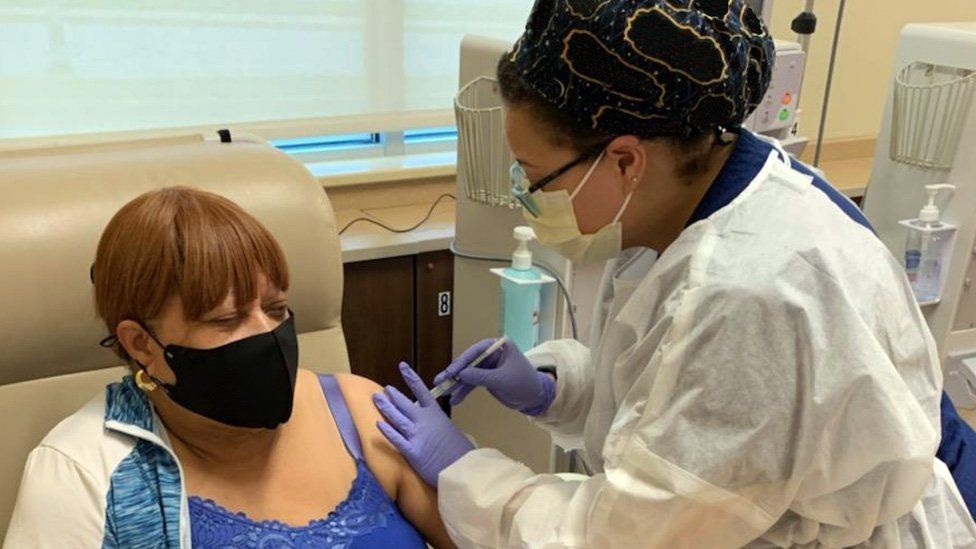

Fearing burnout, but wanting to keep caring for people, in 2021 she became a travelling nurse, giving Covid-19 vaccines. She quickly realised she had a knack for working with people who were anxious or hesitant and had questions – pointing them to the best research and helping them to find the information themselves.
And Henrietta Lacks’s story was always in the back of her mind.
“Knowing what my family history has been, I don’t want anybody else’s family to have that same history. I don’t want them to feel like they were silenced or a silent voice in their care, like Henrietta was.”
For someone who feels personally connected with the darker side of what has been done in the name of science, Victoria knows that simply asking patients to ignore online rumours and trust the science would not be enough.
“I’m never going to try to dance around those hard topics,” she says.
“Yes, these things happened to Henrietta. We’ve come a long way since then. And we are still fighting to make sure that these types of injustices don’t happen now.”
But at the same time Covid was disproportionately affecting the black community, and vaccines were the most powerful tool available to prevent serious illness and death.
Victoria believes in the possibility of acknowledging genuine problems in medicine and the pharmaceutical industry and holding them to account, while also recognising the weight of independent data about a vaccine that has saved an estimated 20 million lives in its first year.
She will explain to her patients how things have changed since Henrietta’s day – including safeguards like the Institutional Review Board, designed to make sure research is conducted ethically, and the need for informed consent.
“We’ve come a long way from 1951. Research has so many checks and balances before they put things out to the public,” she says.
That doesn’t mean there aren’t still issues to solve
Now, as well as her day-to-day work as a nurse and with her family’s initiative HELA100, Victoria is serving as a World Health Organization ambassador for cervical cancer elimination, which she sees as something of a personal mission.
“We know what we know now about cervical cancer because of the loss that my family had to go through,” she says.
It’s another illness that black people in the US are more likely to die of.
Victoria wants as many people as possible to be screened for the HPV virus, to be given access to the vaccine and to early treatment, to bring down deaths from a cancer that is preventable in more than 90% of cases.
“We lost our loved one to cervical cancer,” she says. “But through her death, science was able to come up with the vaccination.”














